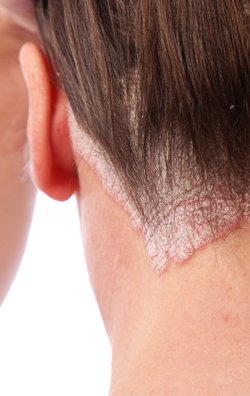
Helicobacter pylori is global, with a prevalence of 30-60% more in developing than in developed countries. Warren and Marshall in Australia in 1983 observed certain spiral, slender bacteria from the gastric mucosa of gastritis and peptic ulcers. Helicobacters colonizes the stomachs of half the human population of the world today!!
They were originally named Campylobacter pylori, which was later renamed as Helicobacter pylori as they differed from Campylobacter in many respects.The only source of H. pylori is the human gastric mucus. The mechanism of transmission is believed to be oral- oral or fecal – oral route. Poverty, poor hygienic conditions and overcrowding favors its transmission. In developed countries, the prevalence H. pylori childhood infections are under control due to improved life style.
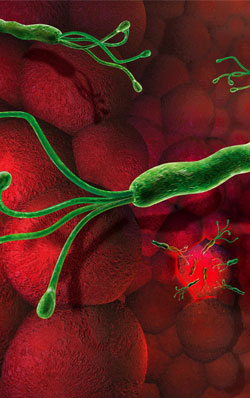
H. pylori is a spiral bacteria which shows considerable motility with the help of a bunch of flagella situated at one end of its body. 5-20% carbon dioxide, pH 6-7 and 37oC favors its growth. It produces hydrogen sulfide and different enzymes like catalase, oxidase, phosphatase and abundant urease. The onset of infection is after an incubation of a few days. H. pylori infections start with mild gastritis lasting for about 2 weeks. In some, the infection may persist for years. Such colonization may be asymptomatic. Even though it might bring about chronic superficial gastritis, it can be demonstrated only through histological examination.
The overlying mucus alone is inhabited and underlying mucosa is not invaded. Gastric antrum is the main place of colonization inside the stomach. The infection is strictly confined to the gastric mucosa and some areas of the duodenum. Bacterial protease, toxins and ammonia are released during the urease activity.
Peptic ulcers are common in affected persons. Later stages are characterized by chronic atrophic gastritis. These may lead to other risk factors for gastric carcinoma like adenocarcinoma and ‘mucosa associated lymphoid tissue’ (MALT) lymphomas. Infection induces the production of IgM, IgG, IgA, etc. but does not seem to provide protection.The genetic mapping of H. pylori reveals that the virulence is associated with certain alleles in the genes, such as cag (cytotoxin associated gene) and vac (vacuolating cytotoxin gene).
Diagnostic tests are of two types;
1. Invasive – involves an endoscopic biopsy of the gastric mucosa, for examination by microscopy, culturing and urease tests. Microscopy is done by silver staining method.Culturing yields good results, but it takes about 3- 7 days.
2. Non invasive – involves serological testing like ELISA and the ‘urease breath test’. In urease breath test, the patient is made to drink a urea solution containing labeled carbon, which can be detected in the breath. It is sensitive and more reliable.H. pylori is sensitive to several antibiotics and also to bismuth salts. The standard treatment is a combination of bismuth subsalicyclate, tetracycline (amoxicillin) and metronidazole for two weeks. An alternative schedule employs a proton pump inhibitor like omeprazole and clarithromycin.Treatment is indicated only for H. pylori related gastric or duodenal ulceration and not foe asymptomatic colonization. Drug resistance and recurrences are common.